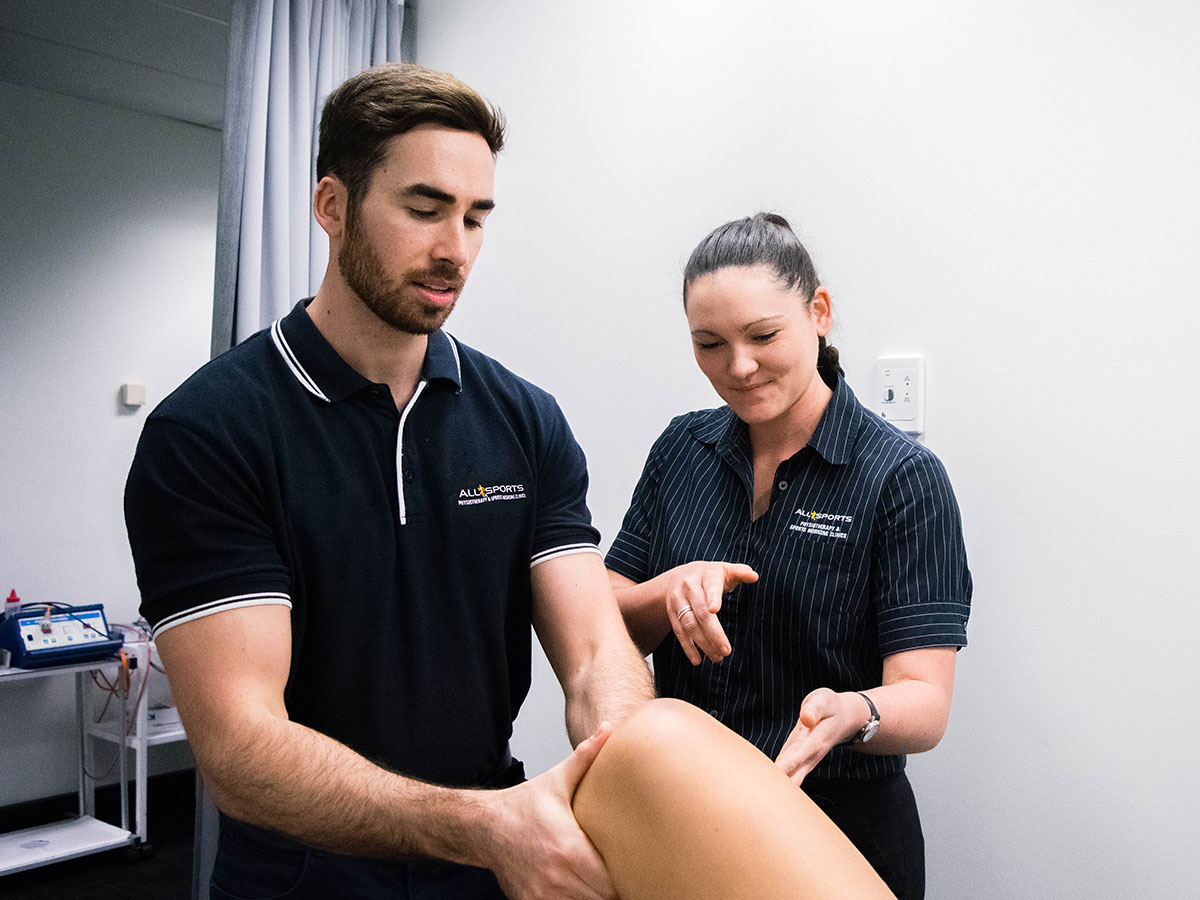

What exactly does a physiotherapist do?
The Allsports Physiotherapy Group is one of the leading providers of allied healthcare in Australia.
We use a multidisciplinary approach to design individualised treatment and rehabilitation programs for a wide range of injuries for patients from all walks of life.
Our growing number of purpose-built physiotherapy and sports medicine clinics provide expert physiotherapy treatment and easy access to a comprehensive range of allied health services aimed at caring for the whole person.
Our Community Partners











